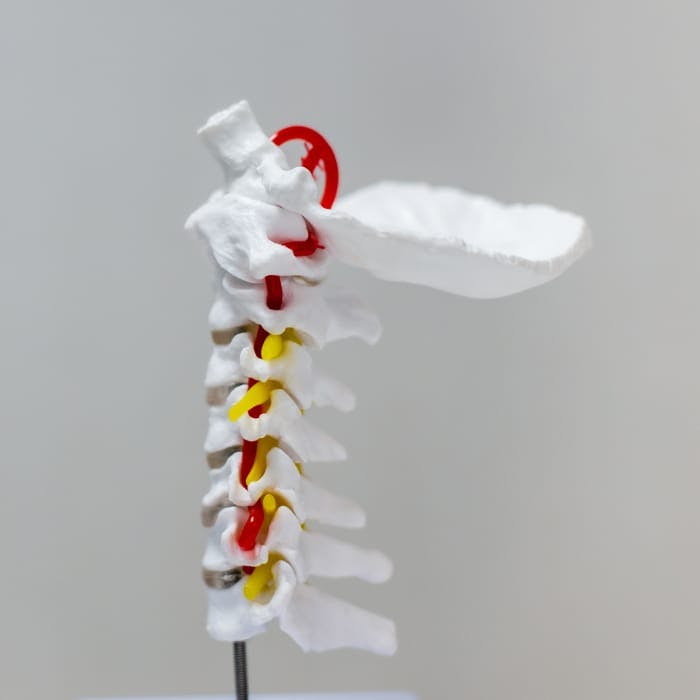
Minimally invasive lumbar discectomy is a surgical procedure performed using specialized instruments inserted through a small skin incision in the lower back to remove part of a herniated disc in the lumbar spine.
Preparing for a Minimally Invasive Lumbar Discectomy
Specific instructions will be provided by your surgeon. In general, you should:
- Inform your surgeon regarding any health conditions, allergies, and medications.
- Avoid smoking as it can slow down the healing process.
- Follow the pre-surgery eating and drinking restrictions.